
11+ Logistics Note Templates in PDF | MS Word
Taking down notes is a common practice on businesses, and it becomes familiar for every worker since note-taking happens even…
Jan 27, 2026
It’s important for nurses to take down note about every interaction that they make with the patients. This is a crucial process because nurses usually administer drugs to the patients during their remainder in the hospital. The records that they have to take down are not as simple as compared to an interview thank-you notes.

However, they are able to manage and handle things, all the while having a small chitchat with the patient, making them feel comfortable and at ease. Some of the things they have to take note of are the patient’s vitals, symptoms, and the medication that needs to be administered, as well as the proper dosage.
Drafting patient documentation can be time-consuming, especially when multiple observations must be recorded accurately during a shift. Using a note maker helps organize vitals, symptoms, medications, and timestamps in a structured and consistent format.
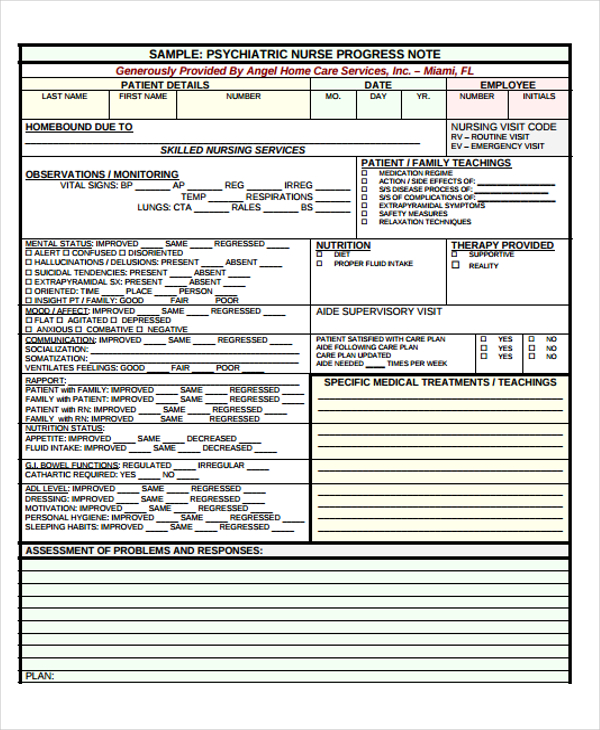
 c.ymcdn.com
c.ymcdn.com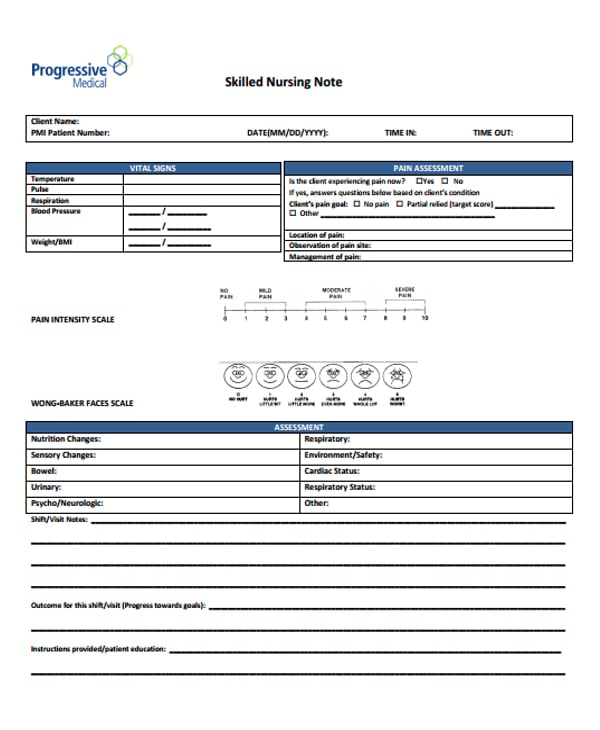 bamamedstaffing.com
bamamedstaffing.com icanotes.com
icanotes.comThe meaning behind the acronym isn’t a complicated one. It’s actually pretty simple and means only the “Subjective, Objective, Assessment, and Plan.” They are a little bit more targeted compared to generic note templates in PDF. Specifically, the job of a SOAP note is to:
Clear and structured note templates help nurses maintain consistent documentation standards across different patient cases and departments. They make it easier to capture clinical details without missing important observations during busy schedules.
Hospice nursing visit is commonly done for those who are terminally ill. But that isn’t always the case, as scenarios would always differ from one another. The nurse on duty, referred to as a hospice nurse, still needs to take notes. There are also some hospice nursing visit note templates in Word. If you want to write one, you can:
Modern AI generators can assist healthcare professionals in organizing nursing observations into clear, well-structured documentation formats while saving time on repetitive formatting tasks. This can be helpful when updating multiple patient notes within a limited timeframe.
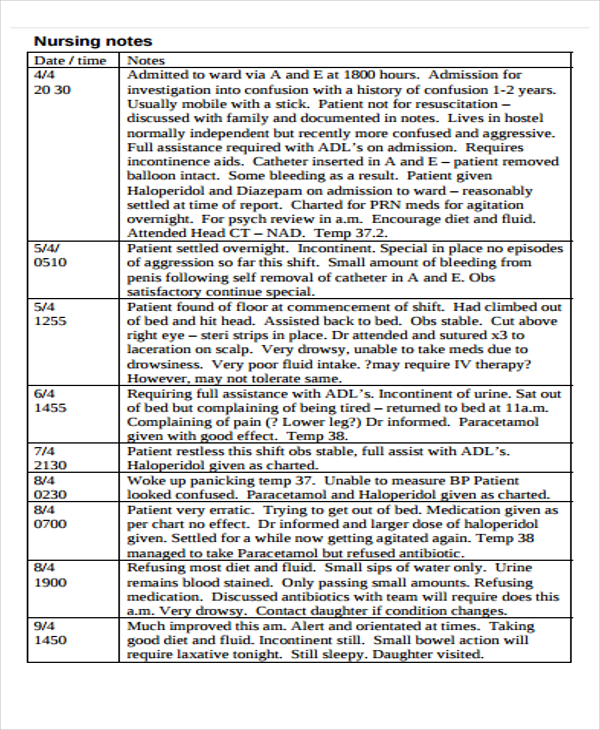 dcn.dementiaelevator.ie
dcn.dementiaelevator.ie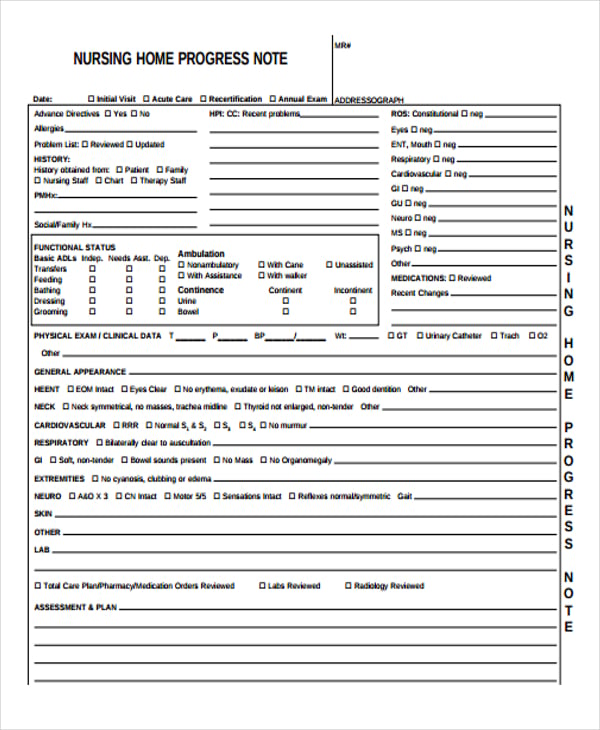 people.virginia.edu
people.virginia.edu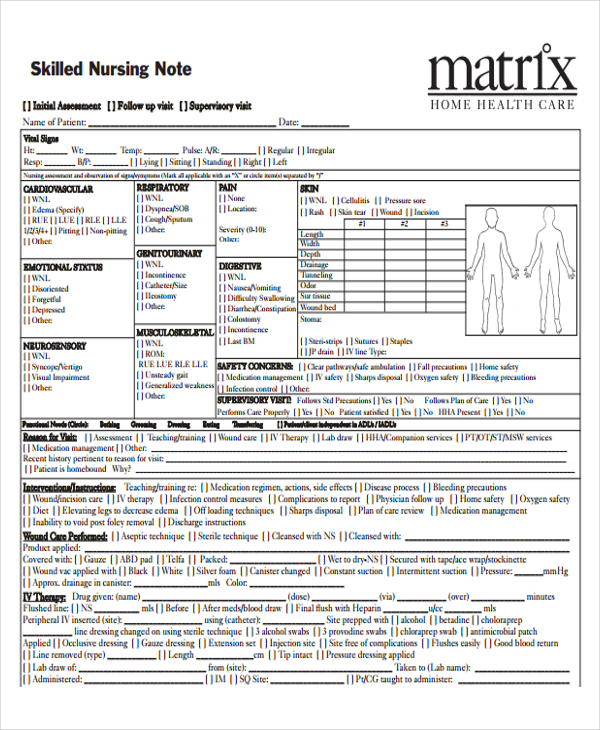 matrixhomecare.com
matrixhomecare.com securityhealth.org
securityhealth.orgWriting is fairly easy when it’s about your thoughts, emotions, and feelings. But writing for nurse notes is a different ball game. Most of the time, you’re writing objectively and taking down notes for the form you need to fill out. If you’re not familiar with what the form looks like, you can check out some free note samples. In order to write some quality nurse notes, you need to:
Starting with free templates allows nurses and healthcare facilities to standardize documentation practices without creating note formats from scratch. This helps maintain accuracy, readability, and consistency in patient records.
Also, you need to double-check if you’re writing it as SOAP note templates. These type of nursing notes differ quite a lot in structure and format, so be sure to study them. Lastly, the secret to a quality nurse note is to be mindful of the situation and accurately detailing everything that’s happening.

Taking down notes is a common practice on businesses, and it becomes familiar for every worker since note-taking happens even…

A printable doctor’s note is a crucial document for employees needing to verify medical absences. It serves as official proof…

A doctor attends to many patients in a day thereby making it difficult to remember the case history of each…

A doctor’s note, or commonly referred to as a medical certificate or sick note, is a verification from a doctor…

An investment promissory note can be referred to as a legal document that compels the person who signs this form…

A credit note is a statement issued and sent to the purchaser by a vendor which certifies that a credit…

A register or a set of notes that is maintained by the audit staff to record some important points observed,…

An absent note is any formally framed letter that’s self-addressed to any senior or body member for not attaining the…

In the simplest of terms, a promissory note refers to a ‘promise to pay.’ In other words, it is a…